Radiation Therapy: Recovery Timeline, Side Effects, and Long-Term Outlook
Radiation therapy is a common cancer treatment that uses high-energy beams to target and destroy cancer cells. Patients considering or undergoing radiation therapy often have questions about how treatment may affect their daily lives, recovery expectations, and long-term outlook. This article provides factual information about radiation therapy, addressing questions about survival after treatment, recovery timelines, and potential side effects without making specific promises about individual outcomes.
Treatment with radiation is often planned in a structured, step-by-step way, but recovery is usually less linear: symptoms can build gradually, peak near the end of therapy, and then improve over weeks. This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Radiation therapy: what recovery often looks like
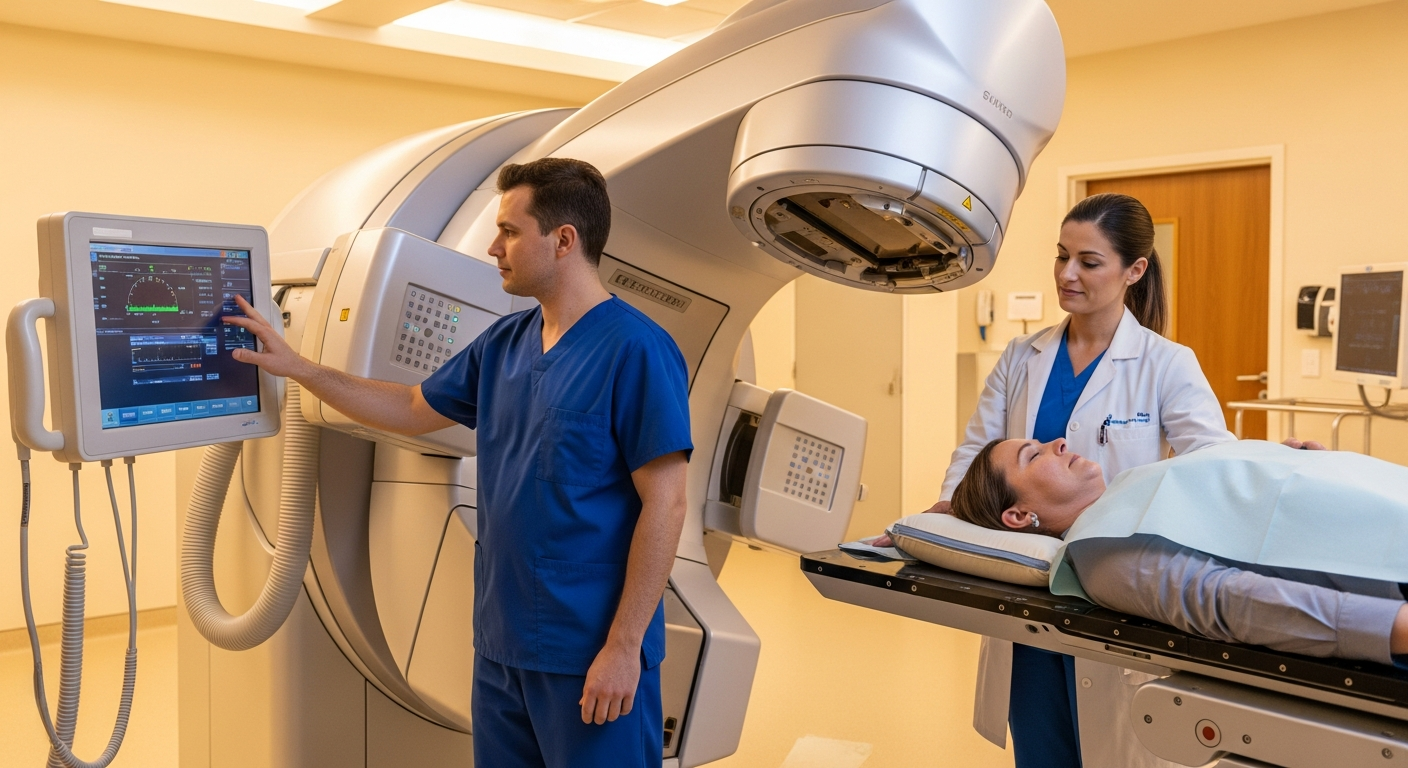
Radiation therapy commonly starts with a planning phase (simulation) followed by daily weekday sessions for a set number of weeks, depending on the goal and treatment site. Many people feel relatively normal at the beginning, with side effects appearing after the first one to three weeks as healthy tissues begin to react. It is also common for symptoms to continue for a short time after the final session, because inflammation can lag behind the last dose.
In many cases, early recovery happens in stages. Acute side effects (those occurring during treatment and shortly after) often begin to ease within two to six weeks. Energy levels may rebound more slowly, especially if treatment is combined with surgery, chemotherapy, or hormone therapy. Clinicians typically schedule follow-ups to check healing, manage symptoms, and confirm whether additional supportive care (nutrition, skin care, pelvic floor therapy, or pain management) is needed.
Photon radiation therapy: how technique can shape side effects
Photon radiation therapy is the most widely used form of external beam radiation in the United States and is delivered by medical linear accelerators. While the goal is always to target the tumor and limit dose to nearby organs, the exact dose distribution depends on planning methods and motion management. Modern approaches such as IMRT (intensity-modulated radiation therapy) and image-guided techniques can help reduce exposure to sensitive structures, which may influence the likelihood or severity of certain side effects.
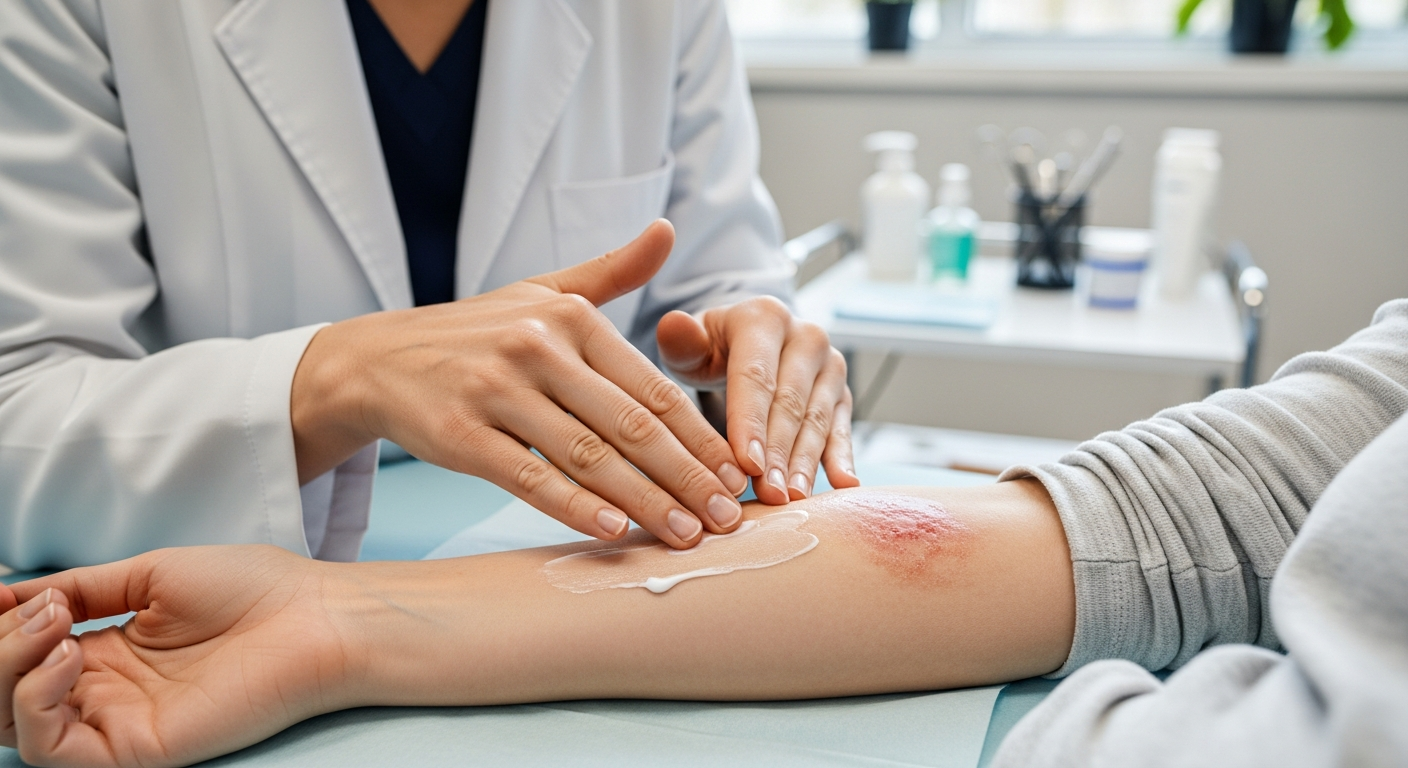
Even with advanced planning, some reactions are tied to the body area treated. For example, skin irritation is more common when shallow tissues are in the field, while digestive or urinary symptoms may occur when the pelvis or abdomen is treated. Asking your care team which organs are considered “at risk” in your plan can clarify what symptoms to watch for, what is expected versus unusual, and what can be treated quickly.
Radiotherapy for prostate cancer: common timeline and recovery notes
Radiotherapy for prostate cancer often involves several weeks of external beam treatments, although some patients may receive different schedules depending on clinical factors and technology. Short-term effects commonly relate to nearby organs, particularly the bladder and rectum. During treatment, people may notice more frequent urination, urgency, a weaker stream, mild burning with urination, or looser stools. These symptoms often build gradually, then improve over several weeks after treatment ends.
Longer-term monitoring matters because some effects can appear months or years later. Your follow-up schedule may include PSA testing and symptom check-ins, along with guidance on pelvic health and sexual function. If hormone therapy is used alongside radiation, it can also affect fatigue, mood, metabolism, and sexual function, so it is helpful to discuss which symptoms are likely attributable to hormone changes versus radiation effects.
Long term effects of chemo and radiation: what to watch for
When chemotherapy and radiation are both part of a treatment plan, it can be harder to separate which therapy is responsible for which symptom. The long term effects of chemo and radiation vary widely based on drug type, radiation site, total dose, age, and other health conditions. Possible long-term issues can include persistent fatigue, changes in bowel or bladder habits, fertility changes (depending on treatment area), neuropathy (more associated with certain chemotherapies), and organ-specific effects such as thyroid dysfunction after neck irradiation.
Another aspect of long-term outlook is survivorship care: managing cardiovascular risk, bone health, cognitive changes, and emotional well-being. Many cancer centers use survivorship plans to summarize past treatments and outline screening and symptom monitoring. If you notice new bleeding, unexplained weight loss, worsening pain, progressive shortness of breath, or neurological symptoms, these should be discussed promptly with a clinician rather than assumed to be a “normal” late effect.
How to find a radiation oncologist in your area
If you are searching for a “radiation oncologist near me,” it can help to think in terms of local services that offer multidisciplinary cancer care, access to modern planning tools, and strong supportive care (nursing triage, nutrition, social work, rehabilitation). Large academic centers and well-established hospital networks may offer a wider range of techniques and clinical trials, while community programs can provide high-quality care with convenience and continuity.
| Provider Name | Services Offered | Key Features/Benefits |
|---|---|---|
| Mayo Clinic | Radiation oncology across many cancer types | Multidisciplinary care teams; multiple U.S. locations |
| MD Anderson Cancer Center | Comprehensive cancer care including radiation oncology | High-volume oncology center; extensive supportive services |
| Memorial Sloan Kettering Cancer Center | Specialized cancer treatment including radiation | Disease-focused expertise; coordinated follow-up care |
| Cleveland Clinic | Oncology and radiation services | Integrated specialty care; broad referral network |
| Johns Hopkins Medicine | Cancer care including radiation oncology | Academic medical center model; coordinated specialty services |
A practical way to compare options is to ask how treatment planning is done (including imaging and motion management), how side effects are handled after hours, and whether your case is reviewed in a tumor board. You can also ask about experience with your diagnosis (for example, prostate cancer workflows), typical appointment cadence, and what support is available for transportation and symptom management.
Recovery after radiation is usually measured in weeks for acute healing and in months to years for long-term monitoring. Understanding the typical timeline, the influence of technique, and the follow-up plan can make the process feel more predictable. While side effects can be disruptive, many are treatable, and a clear communication plan with your care team is one of the most important tools for protecting quality of life over time.